Modern Health Scenario – Trends & Facts
In the 21st Century, the study of public health care has evolved into much more than a need for the medical profession but something that each citizen must comprehend. As countries such as India experience rapid changes economically as well as in terms of their lifestyle choices, there have been some drastic changes in the diseases affecting the people. We are moving away from the purely infective type of diseases and moving towards a scenario where we have the burden of both.
1. Overview of Current Health Figures (India)
The information presented below, compiled from various sources such as ICMR and WHO, points to an increasing trend towards a health crisis situation:
- Diabetes Crisis: Around 11.2% of India’s citizens suffer from diabetes, and the number of people suffering from this disease is well over 100 million.
- Obesity Cases: 28.6% of India’s population is identified as obese, which is a potential cause for metabolic diseases.
- Health Crisis Situations: Air pollution is one of the major causes. A major determinant that helps address this challenge is the Air Quality Index (AQI).
- Lifestyle Issues: Spending too much time on gadgets is causing “Dry Eye Disease” among children, while excessive social media interaction is resulting in loneliness.
Strategic Response: National Programs
As a response to these trends, the government of India introduced the Fit India Movement, which highlights the “Diet Mantra” of proactively cutting back on one’s intake of oil and sugar by 10 percent per day. Additionally, studies indicate that certain behaviors, such as regular washing of hands, could help prevent the spread of infections by up to 50 percent.
The “So What?” Layer:
The environmental and behavioral trends discussed above are considered vital precursors to future health issues. Poor AQI and diets rich in sugar contribute to the foundation of chronic diseases, such as asthma, heart ailments, and Type 2 diabetes. It is necessary to understand these trends to facilitate the transition from a reactive medical approach to a proactive lifestyle one.
2. Re-definition of Health: Holistic Approach
For many years, the prevailing definition of health was “absence of illness”. However, modern-day scientific knowledge and the approach taken by international health authorities indicate that this definition falls short in meeting the demands of our times. The holistic approach is better as it takes into account the fact that a person may have no diseases whatsoever, but still lacks sufficient strength to achieve maximum efficiency.
The WHO Definition of Health
The World Health Organization defines health as a complete state of physical, mental, and social well-being and not just the absence of disease. The holistic approach identifies Three Components of Health:
- Physical Health: The biological performance of the body. The proper functioning of all bodily organs without any disease or injury.
- Mental Health: Refers to a state of psychological balance and a positive outlook. This includes being able to cope with stress and maintain one’s mind clear of negative thoughts.
- Social Health: How effectively an individual interacts socially.
Health versus “Not Sick”
The differentiation between health and “not sick” is essential. While an individual who is “not sick” may not have any recognized ailments, he might be devoid of energy to function effectively in his day-to-day life. On the other hand, a healthy individual completes his responsibilities more effectively and has the ability to survive under immense pressure. Health can be defined as the ability to adapt oneself to the surroundings.
The holistic perspective of health is remarkably similar to our ancient scientific knowledge.
3. Scientific Legacy: Ayurveda and Prevention-Oriented Lifestyle
The strategic importance of traditional medical approaches like Ayurveda, Siddha, and Unani medicine is becoming more and more clear in terms of modern preventive strategies. In contrast to conventional medicine, which emphasizes treatment over prevention, traditional medicine stresses the need to keep healthy rather than getting sick.
Basic Principles of Ayurveda Medicine
According to Ayurveda, health is always about the balance between your body, soul, and the environment. The main ideas include:
- Dincharya (daily regimen): Strict daily regime from morning until bedtime.
- Ritucharya (seasonal regimen): Adjustment of lifestyle according to seasonal changes. For instance, the human organism needs more sleep in winters or some kind of clothing adaptation due to certain season.
- Prakriti (nature constitution): Everybody has his or her own nature. One’s diet should depend on it. For instance, an athlete needs protein foods because of physical loads, whereas a student requires other kinds of products for intellectual work.
Elements of a Healthy Lifestyle
- Healthy Eating: Emphasis on Whole Grains (keeping the bran and germ intact) rather than Refined Grains (stripped of nutrients).
- Personal Hygiene & Sanitation: Keeping oneself clean to prevent exposure to germs.
- Sufficient Rest/Sleep: Vital for bodily healing and mental restoration.
- Mind-Body Techniques: Employing Yoga, Meditation, and Mindfulness for mental calmness and focus.
Although these preventative measures serve as the first step in disease prevention, the clinical diagnosis of any disorder is imperative once the balance is disturbed.
4. Clinical Indicators: Distinguishing Between Symptoms and Signs
The success of a medical procedure hinges on the knowledge of clinical indicators. The patient’s appropriate medical care can be guaranteed through the proper identification of symptoms and signs.
Symptoms versus Signs
| Factor | Symptoms | Signs |
| Description | Experiences known only to the patient and not visible to others. | Observable characteristics, which can be quantified by a healthcare professional. |
| Characteristics | Cannot be identified by an observer. | Can be perceived or measured by an observer. |
| Illustrations | Pain, dizziness, fatigue, nausea. | High body temperature, rashes, swollen areas, high blood pressure. |
It is important to understand this difference in the diagnostic process. Symptoms give the physician insight into the internal state, whereas signs enable him/her to diagnose a specific disease.
5. Categorization of Diseases: Communicable and Non-Communicable Diseases
Diseases are divided according to their biological origin and the impact they have on human society.
Two Main Types
- Communicable (Infectious) Diseases: Are biologically caused and come from biological agents (bacteria, viruses, fungi, protozoa, and worms). These diseases may travel between hosts.
- Examples: Influenza, Typhoid, COVID-19, Chicken Pox.
- Non-Communicable Diseases (NCDs): These diseases are not biologically caused by any organisms. These diseases arise out of genetic factors, environments, or behavioral choices of individuals.
- Examples: Diabetes, Cancer, Asthma, Deficiency diseases like anemia.
Chronic Diseases
The majority of NCDs fall under the category of chronic diseases. A chronic disease lasts more than three months. Therefore, treatment approaches must move from cure to management. The reason why management is necessary is that these diseases are caused by deep-set changes in biology or the environment. As such, chronic diseases require a different approach to management since the agent responsible for the disease is not an invader but something internal.
Once a disease is recognized as communicable, the next step would be the identification of mechanisms used to transmit the disease.
6. Methods of Transmission: Pathogens & Vectors
The transfer of infectious agents occurs along unseen routes. The detection of these routes becomes critical to the erection of public health barriers.
- Air-borne: Pathogens are discharged in droplets either by coughing or sneezing (e.g., Common Cold, Tuberculosis).
- Water/Food-borne: Transmission by ingesting contaminated supplies (e.g., Cholera, Typhoid, Hepatitis A).
- Vector-borne: Pathogens are transported from one host to another through insects called vectors. As examples, the Female Anopheles mosquito acts as the vector for Malaria, while the Aedes mosquito serves as the vector of the Dengue virus.
- Contact Transmission: Either direct or indirect transmission through skin contact or sharing of personal effects like towels.
- Rabies in Animals: Some specific viruses such as Rabies are spread through the saliva of rabid animals (e.g., dogs, foxes) through bites or wounds.
Parasites: Certain pathogens such as Roundworms act as parasites within the human digestive system. These pathogens extract nourishment from their hosts, resulting in stunted growth, malnutrition, and anemia.
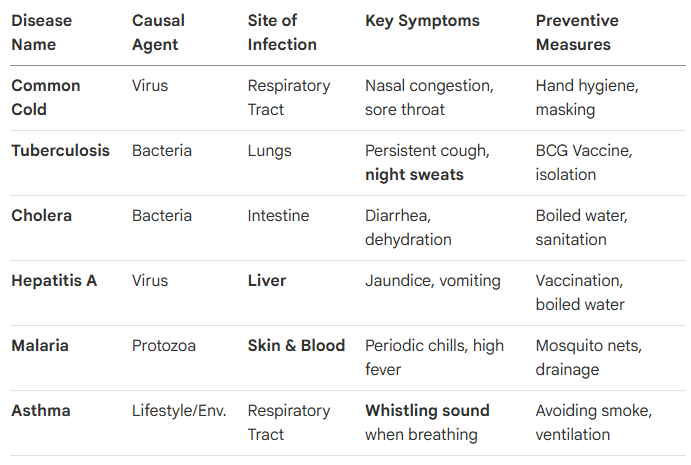
7. Deep Dive: Common Diseases and Prevention (Reference Table)
Strategic prevention requires tailoring measures to the specific pathogen and its site of infection.
Common Communicable and Non-Communicable Indicators
Sanitation Strategy: The Example of Odisha
The community-based strategy on sanitation in Bhadrak, Odisha, is a fine example of the potential of environmental management. Through the construction of latrines and lowering the levels of open defecation, the community has managed to minimize food and water contamination and consequently the incidence of diarrhea.
8. Defense and Science: Immunity and Vaccination
The human body contains its own “Internal Army” called the Immune System, which identifies and attacks foreign invaders or harmful pathogens.
Natural Immunity versus Acquired Immunity
- Natural Immunity: An innate capacity to combat all kinds of infections, starting right from birth.
- Acquired Immunity: Immunity gained due to prior exposure to a particular microbe or vaccines; acquired immunity is a “learned” response.
How Vaccines Work
Four main approaches are used to train the immune system through vaccination:
- Dead Pathogens: Inactivated microbes introduced into the body (example, Polio).
- Weakened Pathogens: Live yet attenuated microbes (example, BCG for Tuberculosis).
- Inactivated Parts/Toxins: Introduction of only the toxin of the pathogen (example, the toxic part of the Tetanus bacteria).
- Genetic Instructions: Modern-day vaccines, such as those against the Coronavirus, which instruct cells to manufacture an inactive part of the organism.
History Highlight
The science of vaccinating began with Edward Jenner, who used Cowpox to develop the first vaccine for Smallpox. However, thousands of years before Jenner, Indian doctors used “Variolation” (Tikekaras), where patients were intentionally exposed to mild Smallpox substances.
9. Medical Interventions: Antibiotics and the Resistance Crisis
Whereas vaccines are preventive, medical intervention is essential for curing existing cases of infection.
Penicillin Discovery
In 1928, Alexander Fleming discovered Penicillin from a mold (Penicillium) that killed bacteria. Antibiotics operate on structures present in bacteria such as the cell wall, but which are not present in human body cells. It is worth noting that antibiotics are completely useless when combating viruses since viruses do not have these structures.
CRITICAL: The Antibiotic Resistance Crisis
The ‘so what’ about modern medicine today is antibiotic resistance. Over prescription, for example, when an individual uses antibiotics for cold viruses, stops medication before completion or excess consumption among livestock breeds bacteria with resistance. Consequently, these survivors develop into “Superbugs” making infections untreatable.
Indian Pioneers
- Dr. Kamal Ranadive: Has pioneered biomedical research that links hormones, viruses to causing cancer.
- Dr. Maharaj Kishan Bhan: Has been the Secretary of the Department of Biotechnology; played a key role in developing a Rotavirus vaccine that protects children from diarrheal diseases.
In conclusion, be it ancient or modern preventive health measures, the dictum still applies: prevention is better than cure. Simple hygiene practices, for example, washing hands regularly can significantly lower infection rates by fifty percent.